What is the vagus nerve?
The vagus nerve is the main component of the parasympathetic nervous system, which is responsible for bodily functions during rest – it keeps your body working as intended[1]. The vagus nerve begins at the base of the brain and goes through the heart, lungs, digestive tract, and abdomen. This nerve has a number of functions, including initiating your automatic responses to perceived threats (or safety). It’s why your heart races or stomach tightens when you’re feeling scared or stressed[2].
The vagus nerve has both direct and indirect connections to groups of neurons and synapses that are involved in emotional and cognitive functions. These are the same groups of neurons and synapses that are hindered by depression. Evidence shows that stimulating and strengthening the vagus nerve can reduce the symptoms associated with mental health challenges.
What is vagus nerve stimulation?
Vagus nerve stimulation (VNS) involves using a small, surgically implanted device to stimulate the vagus nerve with electrical impulses. VNS is primarily used to treat epilepsy but there is promise for its effectiveness in depression treatment. It is currently FDA-approved for adults who have treatment-resistant depression (TRD), haven’t improved after trying four or more medications or electroconvulsive therapy (or both), and say they will continue standard depression treatments along with VNS[3].
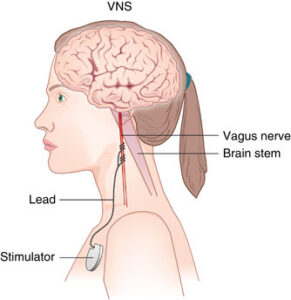
VNS begins with a surgical procedure in which a battery-powered device about one and a half inches across is placed under the skin on the chest. A wire is threaded under the skin from the chest up to the neck, connecting the device to the left vagus nerve. The device is activated by a doctor after surgery and programmed to send electrical impulses to the vagus nerve at different durations, frequencies, and currents. These signals travel along the vagus nerve to the brainstem, which in turn sends signals to specific areas of the brain, including those that affect mood[4].
How can VNS treat mental health conditions?
Brain imaging studies in humans have shown that VNS influences activity in the same brain regions that depression impacts. Additional animal and human studies have shown that VNS influences the activity of norepinephrine, serotonin, and other neurotransmitters involved in mood disorders[5]. Similar to antidepressant medications, VNS also increases the expression of Brain-Derived Neurotrophic Factor (BDNF), a molecule associated with resilience and stress tolerance[6].
How effective is VNS?
The efficacy of VNS as a treatment for depression is still being researched. Most studies have found that the benefits of VNS take time to set in – it may take several months of treatment before there are noticeable improvements in depressive symptoms[7].
- In the studies that led to the 2005 FDA approval of VNS for TRD, there was no benefit during the first two to three months of treatment. After one year, 20-30% of patients saw significant improvements in their symptoms, while others saw no improvement, or their symptoms worsened[8].
- A five-year study of 795 patients with TRD found that those treated with VNS had better clinical outcomes than the treatment-as-usual (TAU) group. The VNS group had a significantly higher five-year response rate (67.7% compared to 40.9%) and remission rate (43.3% compared to 25.7%)[9].
- A 2020 study of individuals with treatment-resistant bipolar depression (TRBD) found that 63% of those treated with VNS in addition to TAU had a significant reduction in depressive symptoms, compared to 39% of the TAU group[10].
Is VNS safe?
Research on VNS does not show any major safety concerns, but there are some risks, as there are with any medical procedure. Surgical complications are rare and similar to other types of surgery, like soreness at the incision site and risk of infection. People also experience some side effects from the implanted device, like voice changes, throat pain, or difficulty swallowing. For most people, these side effects are minor, tolerable, and lessen over time. In some cases, the side effects bother people for as long as they continue with VNS, though adjusting the electrical impulses can help reduce side effects. It is possible to shut off the device temporarily or permanently if the side effects aren’t tolerable or outweigh the benefit of VNS[11].
[1] Nall, R. (2020, April 23). Your parasympathetic nervous system explained. Healthline. https://www.healthline.com/health/parasympathetic-nervous-system
[2]Psychology Today. (2019, June 13). Vagus nerve. https://www.psychologytoday.com/us/basics/vagus-nerve
[3] Mayo Clinic. (2020, November 17). Vagus nerve stimulation. https://www.mayoclinic.org/tests-procedures/vagus-nerve-stimulation/about/pac-20384565
[4] Mayo Clinic. (2020, November 17). Vagus nerve stimulation. https://www.mayoclinic.org/tests-procedures/vagus-nerve-stimulation/about/pac-20384565
[5] Howland, R.H. (2014). Vagus nerve stimulation. Current Behavioral Neuroscience Reports, 1(2), 64-73. doi: 10.1007/s40473-014-0010-5
[6] Notaras, M. & van den Buuse, M. (2020). Neurobiology of BDNF in fear memory, sensitivity to stress, and stress-related disorders. Molecular Psychiatry, 25, 2251-2274. doi: 10.1038/s41380-019-0639-2
[7] Mayo Clinic. (2020, November 17). Vagus nerve stimulation. https://www.mayoclinic.org/tests-procedures/vagus-nerve-stimulation/about/pac-20384565
[8] American Association of Neurological Surgeons. (2010, July 14). Vagus nerve stimulation. https://www.aans.org/en/Patients/Neurosurgical-Conditions-and-Treatments/Vagus-Nerve-Stimulation
[9] Aaronson, S.T., et al. (2017). A 5-year observational study of patients with treatment-resistant depression treated with vagus nerve stimulation or treatment as usual: Comparison of response, remission, and suicidality. The American Journal of Psychiatry, 174(7), 640-648. https://doi.org/10.1176/appi.ajp.2017.16010034
[10] NeuroNews International. New study shows significant positive impact of vagus nerve stimulation therapy for treatment-resistant bipolar depression. https://neuronewsinternational.com/vagus-nerve-stimulation-for-depression/
[11] Mayo Clinic. (2020, November 17). Vagus nerve stimulation. https://www.mayoclinic.org/tests-procedures/vagus-nerve-stimulation/about/pac-20384565

